When the world was going through the pandemic of smallpox in the 18th century in the whole of Europe it was first seen by Edward Jenner that milkman was not getting infected by smallpox disease even after exposure to the infection for a long time. By seeing this Edward Jenner thought that something in the body is protecting them from deadly smallpox. After a close observation, he found out that the milkmen were previously infected by cowpox disease which was the reason for which they were not affected with smallpox.
The thing was therefore named vaccine as Vacca in Latin meant cow. The vaccination technique then started in whole Europe where the inoculation of the cowpox virus was used as vaccines to prevent the population from smallpox. And in around the next 100 years all around the globe, smallpox was completely eradicated. We have come a long way from there. Diseases like polio which were completely fatal are on the verge of eradication in the world due to successful government vaccination programs.
How a vaccine works
To know how a vaccine works we have to go deep down about how our immune system works against an antigen. Our immune system is composed of many types of cells like t lymphocytes, b lymphocytes, and macrophages. Each has different functions to protect the body. Some produce antibodies that destroy the pathogens, some produce toxins and some carry out phagocytosis. The immune system also stores its encounters as memories which are used later on when the same pathogen is encountered.
But sometimes the pathogen causes so much damage on its first time of infection that the human being dies. These infections are nearly fatal like polio, smallpox, measles, etc. For this, the body needs to be ready to fight the infection. The vaccines are mostly weakened or dead form of the virus that is completely safe for the body. The vaccine teaches the immune system how to make antibodies against the pathogen and kill it. A vaccine is safe and effective when approved because it has to go through rigorous clinical and lab trials to study its toxicity side effects and efficacy.
TYPES OF VACCINE
Vaccines are of multiple types and are made according to how the immune system responds to the germ. Based on these vaccines can be of the following types-
- Messenger RNA (mRNA) vaccines
- Subunit, recombinant, polysaccharide, and conjugate vaccines
- Toxoid vaccines
- Viral vector vaccines
- Live-attenuated vaccines
Each type of vaccines work in different ways.
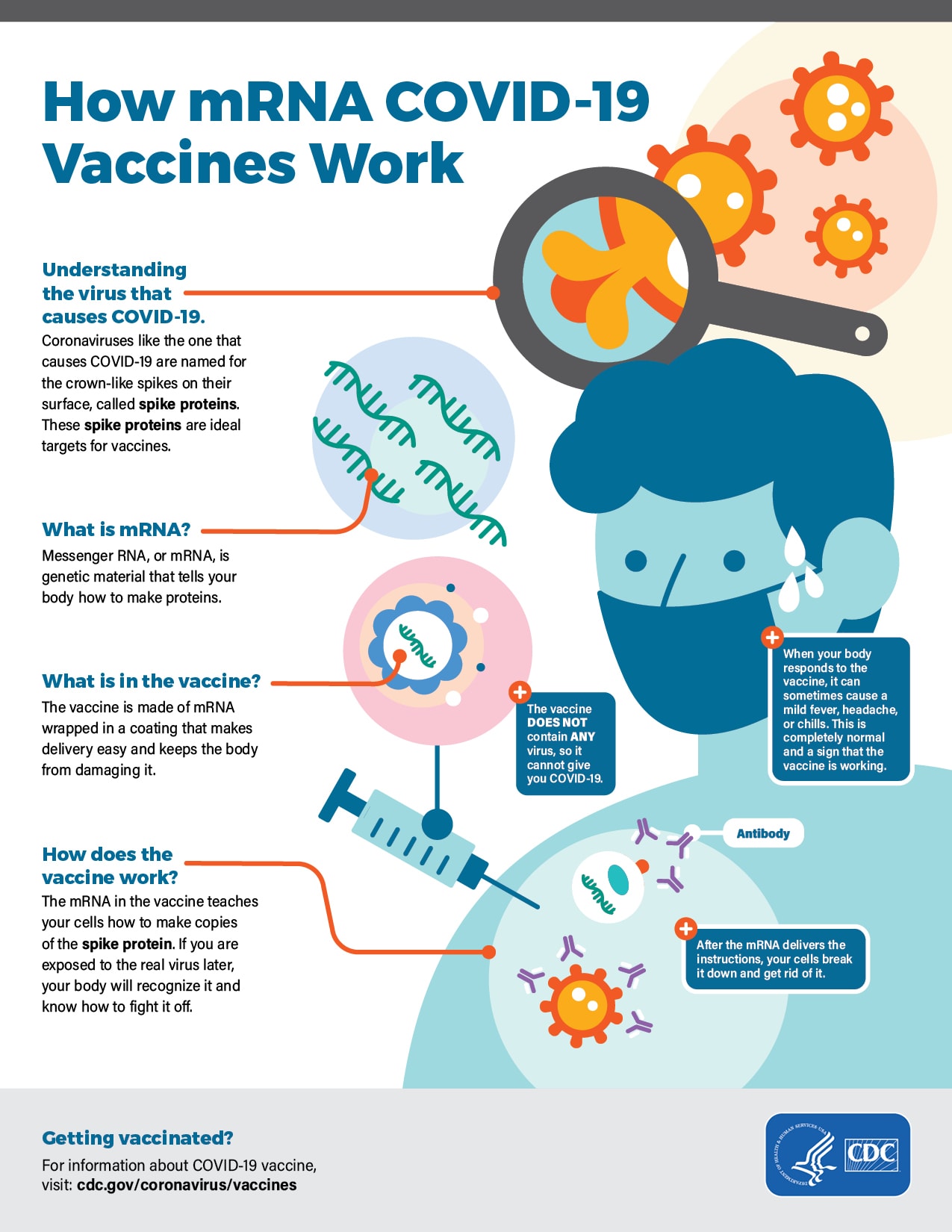
mRNA vaccines
mRNA (messenger Ribose Nucleic Acid) is the RNA that codes for proteins by a process called translation. In other words, they can be termed as the median in between DNA to proteins.
Pfizer and Moderna are MRNA type vaccines. mRNA vaccines are the newest technology used for making vaccines. These vaccines have certain advantages over their counterparts like they are quick to make and as they do not contain any virus itself they have no risk of causing the disease.
mRNA vaccine is based on the principle of teaching the immune system how to make certain proteins required fighting with the pathogen. The proteins are called antibodies.
The first mRNA vaccine in the world that was approved for use was made by Pfizer against the deadly coronavirus. It is a two-shot vaccine given at an interval of 3 weeks (21 days).
These mRNA-based vaccines are also considered safe as they do not get inside the nucleus of the cell and get destroyed after their task is completed.
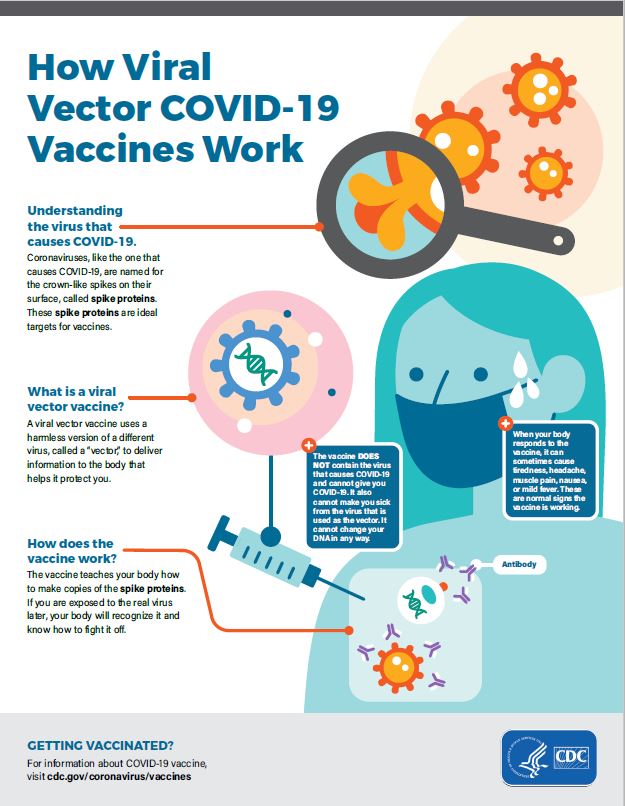
Viral vector vaccines
These vaccines are Viral vector-based vaccines that differ from most conventional vaccines in that they don’t contain antigens, but rather use the body’s cells to produce them. They do this by using a modified virus (the vector) to deliver genetic code for antigen, in the case of COVID-19 spike proteins found on the surface of the virus, into human cells. By infecting cells and instructing them to make large amounts of antigen, which then trigger an immune response, the vaccine mimics what happens during natural infection with certain pathogens – especially viruses. This has the advantage of triggering a strong cellular immune response by T cells as well the production of antibodies by B cells. An example of a viral vector vaccine is covshield by AstraZeneca and Johnson and Johnson vaccine. These vaccines are also more effective against the pathogen causing the disease but its making takes an ample amount of time. High-scale productions in factories take lots of time and require big pharmaceutical machinery and multiple types of raw materials. Suspension cell lines are necessary to grow these viral vectors in bioreactors.
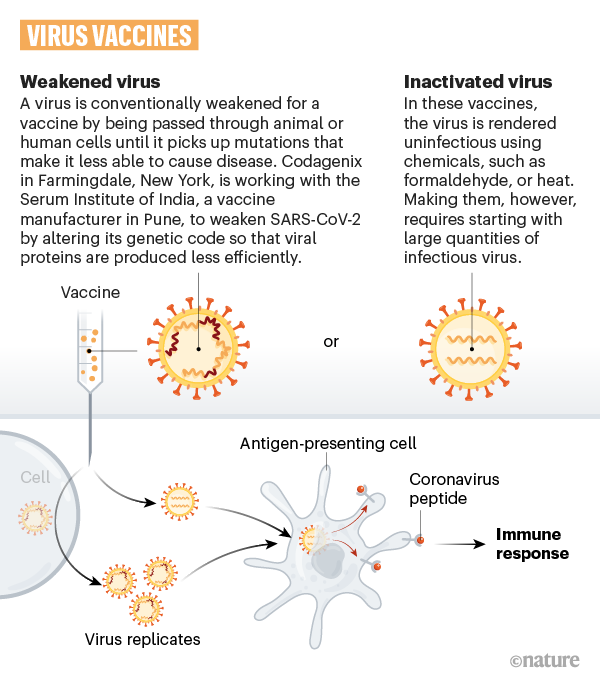
Inactivated virus vaccine
These vaccines have the virus itself for triggering the immune response but in such a form that it cannot case. The real disease Inactivated vaccines use the killed version of the germ that causes a disease.
Inactivated vaccines usually don’t provide immunity (protection) that’s as strong as live vaccines. So you may need several doses over time (booster shots) to get ongoing immunity against diseases. Some example of inactivated virus vaccine is covaxin by Bharat biotech and coronavax and sinopharm vaccine by china.
As they mostly use inactivated virus for their vaccine their manufacturing time is a bit less than the other vaccine types.
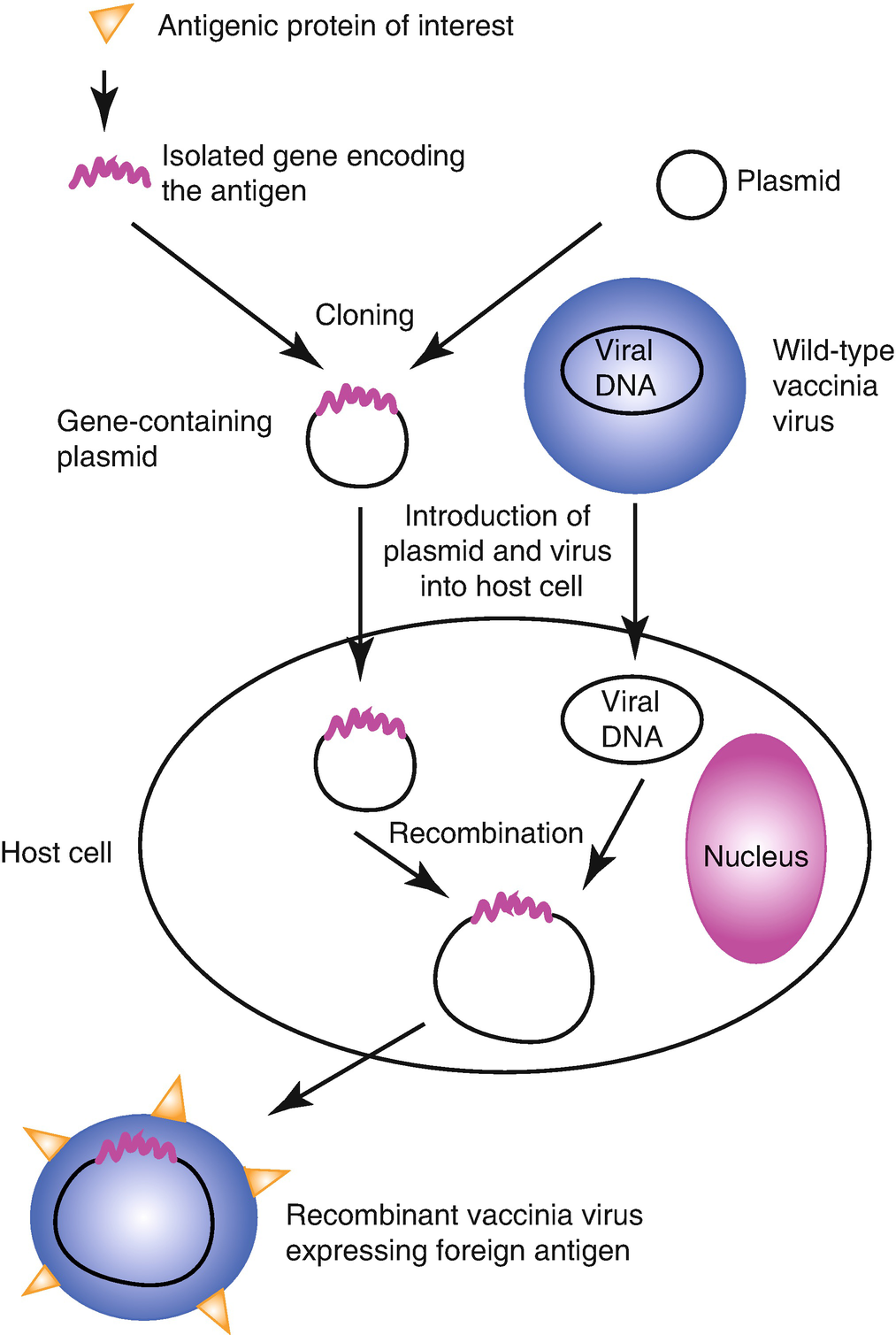
Subunit, recombinant, polysaccharide, and conjugate vaccines
Subunit, recombinant, polysaccharide, and conjugate vaccines use specific pieces of the germ—like its protein, sugar, or capsid (a casing around the germ).
Because these vaccines use only specific pieces of the germ, they give a very strong immune response that’s targeted to key parts of the germ. They can also be used on almost everyone who needs them, including people with weakened immune systems and long-term health problems.
One limitation of these vaccines is that you may need booster shots to get ongoing protection against diseases.
An example of this type of vaccine is novovax which is a protein-based vaccine based on the spike proteins of the virus.
REFERENCES
https://www.bbc.com/news/world-asia-india-55748124
https://www.vaccines.gov/basics/types
https://en.wikipedia.org/wiki/Lymphocyte
https://www.nature.com/articles/nrd.2017.243
https://www.nature.com/articles/d41586-020-00502-w
https://www.cdc.gov/coronavirus/2019-ncov/vaccines/different-vaccines/mrna.html
https://link.springer.com/chapter/10.1007/978-3-030-00710-2_14














