Radiotherapy is a foundation of both therapeutic and palliative cancer care. In any case, radiotherapy is seriously restricted by radiation-induced toxicities. In the event that these toxicities could be reduced, more doses of radiation could be given consequently encouraging a better tumor reaction.
Initial pre-clinical examinations have shown that irradiation at dose rates far surpassing those presently utilized in clinical settings lessen radiation-induced toxicities while keeping a comparable tumor response. This is referred to as the FLASH effect. Until now, just a patient has been exposed to FLASH radiotherapy for the treatment of subcutaneous T-cell lymphoma bringing about minimal toxicities and complete response.
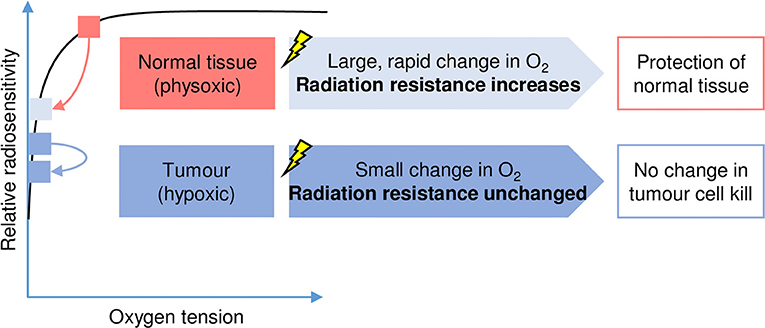
The instrument responsible for diminished tissue responsible following FLASH radiotherapy is yet to be explained, however, the most noticeable speculation so far proposed is that acute oxygen depletion happens within the irradiated tissue. This survey examines the tissue response to FLASH radiotherapy, basically assesses the proof supporting speculations surrounding the biological source of the FLASH effect, and believes the potential for FLASH radiotherapy to be converted into clinical settings.
What Purpose Does Flash Ultra-high-dose Rate Radiation Therapy Serve?
The research group has expanded to involve medics in clinical radiation oncology and dermatology, creating what they believe will be the first human safety trial with FLASH radiotherapy at Dartmouth-Hitchcock, treating patients with advanced skin lesions that cannot be removed surgically.
Although, radiotherapy forms part of the treatment of cancer, however, it additionally harms the healthy tissue surrounding the tumor. The success of the treatment is subject to conveying a sufficiently high dose of radiation to destroy the tumor cells without making extreme injury to the surrounding tissues.
FLASH radiotherapy (FLASH-RT) is another strategy, involving the treatment of tumors at super high dose rates which really reduces the injury to ordinary tissue around the tumor while equalling the anti-tumor effect of conventional-dose rate radiotherapy (CONV-RT). Notwithstanding, just a little is known about the components behind the FLASH impact.
How Was The First Patient With FLASH-radiotherapy Treated?
In 2019, A 75-year-old patient had multiresistant CD30+ T-cell cutaneous lymphoma spread all through the entire skin surface. Localized skin RT was previously utilized more than 110 times for different ulcerative or potentially agonizing cutaneous lesions advancing regardless of systemic treatments.
Nevertheless, the tolerance of these RT was naturally poor, and it was assumed that FLASH-RT could deliver an equivalent tumor control probability while being less harmful to the skin. This
treatment was given to a 5.6-MeV linac with a 3.5-cm width skin tumor precisely intended for FLASH-RT. 15 Gy in 90 ms was the prescribed dose to the PTV. Excess dosimetric estimations were performed with GafChromic films and alanine, to review the consistency between the delivered and the prescribed portions.
The peak of the reactions at three weeks, a grade one oedema (CTCAE v 5.0) alongside a transient grade one epithelitis (CTCAE v5.0) in delicate tissues surrounding the tumor were noticed. Clinical assessment was compatible with the optical coherence tomography indicating no lessening of the thickness of the epidermis and no disorder at the basal layer with a limited increment of the vascularization.
The tumor response was quick, finished, and strong with a short follow-up of 5 months. These perceptions, both on the skin and the tumor, were promising and prompt to additional clinical assessment of FLASH-RT.
Scientists Created FLASH Ultra-high-dose Rate Radiation Therapy Beam For Cancer Treatment
A joint group of scientists from Dartmouth Engineering, and Dartmouth-Hitchcock’s Department of Surgery, Radiation Oncology at Dartmouth’s and Dartmouth-Hitchcock’s Norris Cotton Cancer Center (NCCC) developed a technique to change over a standard linear accelerator (LINAC), utilized for delivering the treatment of radiation therapy cancer, to a FLASH ultra-high-dose rate radiation therapy beam.
The extraordinarily high dose rate is multiple times higher than ordinary therapy treatment. Recently, the FLASH beam is being utilized in preclinical researches on both experimental animal tumors just as in clinical veterinary medicines, to study the normal effects of the tissue-sparing and how to maximize the value.
Reference:
- https://www.frontiersin.org/articles/10.3389/fonc.2019.01563/full
- https://www.google.com/amp/s/www.news-medical.net/amp/news/20210119/Researchers-develop-FLASH-ultra-high-dose-rate-radiation-therapy-beam-for-cancer-treatment.aspx
- https://www.google.com/amp/s/researchoutreach.org/articles/flash-radiotherapy-what-how-why/amp/














